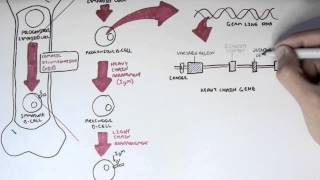
the immune response is highly specific for each Invader and that's because the cells of the Adaptive immune response have receptors that differentiate one pathogen from another by their unique Parts called antigens the key cells of the Adaptive immune response are the lymphocytes the B and T cells which have unique antigen receptors known as the B cell receptor or BCR and T Cell receptor or TCR respectively both B cells and t- cells undergo a process called vdj rearrangement to generate a massively diverse set of receptors B cells can further enhance the diversity of their BCR repertoire
using a process called somatic hypermutation and the result is that the cells that emerge will have a stronger and more specific response to the antigen and this is called Affinity maturation now remember that the B cell receptor is essentially an antibody except that it's attached to the surface of the B cell and each B cell receptor or antibody has two general Parts the variable region which binds antigen and the constant region which determines the specific antibody class IGM IG IG igd or IG first let's start with the activation of B cells which occurs when a
foreign antigen binds and cross- links adjacent bcrs thereby triggering a Cascade of events that help B cells proliferate and differentiate once activated the B cell internalizes the antigen and presents a piece of it on a major histo compatibility complex Class 2 molecule or MHC Class 2 for short at some point along comes a CD4 positive helper t- cell that binds to the presented antigen when this interaction occurs the t- cell expresses a protein called cd40 Li on its surface which binds to the the cd40 receptor on the B cell this triggers a series of events
that eventually result in the activation of the enzyme called activation induced citadine deaminase or aid for short this enzyme is only found in B cells and allows them to make Cuts in the DNA causing the B cell to class switch from IGM to ig IG or IG at the same time the t- cell secret cyto kindes that bind cyto kind receptors on the B cell providing Specific Instructions on what class of antibody it should start producing because of the role that Aid plays in class switching people who lack Aid suffer from a condition known as
Hyper IGM imuno deficiency where they have a hard time making antibodies other than IGM the most common cause of this condition is an xlin recessive genetic defect of the cd40 Lian that leaves helper T cells incapable of binding cd40 receptors on B cells in addition to promoting class switching Aid also leads to sematic hypermutation somatic hypermutation only happens in activated B cells not t- cells and primarily occurs in the germinal centers of the lymph nodes and spleen you see Aid can only bind to single stranded DNA so it's really only able to Target genes that
are being actively transcribed during the rapid proliferation phase that occurs following B Cell Activation the way the aid enzyme works is turning a citadine into a urine in the DNA now keep in mind that urine is completely foreign to DNA and typically only found in RNA and urine can't properly bind to the guanosine nucleoside on the opposite DNA strand as a result the cell tries to fix this mistake in the DNA in one of two ways either mismatch repair or Bas exision repair in mismatch repair the mismatch repair proteins msh2 and msh6 wooin to fix
the DNA before transcription is complete they kind of do this like the pit crew at a NASCAR race trying to quickly fix a car on lap 40 out of 100 msh2 and msh6 recruit nucleases which remove the urine and several adjacent nucleotides from the DNA and then DNA polymerase comes in to help replace the nucleotides this process is extremely aerop prone and tends to introduce mutations into the DNA the other option is base exision repair which is where the enzyme uracil DNA glycosylase removes the uracil base from the urine and typically in the next round
of DNA replication a random nucleotide is inserted into the opposite DNA strand by DNA polymerase once again leading to a mutation and these random mutations mean the daughter cells of the initial b cell may have a very different antigen specificity than their mother cell now even though random mutations in a gene are usually a problem mutations in the variable region of the BCR are actually a really good thing that's because the changes affect how strongly the BCR binds to the antigen it's affinity for the antigen and since the B cells will eventually become plasma cells
that secrete antibodies this process affects the antibody affinity for antigen while some daughter cells have mutations in their BCR that increase the affinity for antigen others have mutations that decrease it if a b cell's Affinity is so low that it doesn't respond to the antigen anymore then the B cell will simply stop getting activated and will die out over time meanwhile other cells will get a stronger and stronger Affinity over the generations and this is what leads to Affinity maturation it's really like natural selection on a cellular level sped up so that we see changes
happening over days instead of over thousands of years while all of this is happening keep in mind that there's an immune IM response taking place and that there's initially lots of antigen floating around over time as the immune system clears away more and more of the infection there's less antigen left for this process of affinity maturation that means that only the bcrs with the highest affinity for the antigen will be able to bind to the small amount that's floating around in other words as antigen is removed it helps to also promote only the daughter cells
with bcrs that have the strongest ability to bind the antigen and mount a response against it all right as a quick recap somatic hypermutation only occurs in B cells which express the enzyme aid aid is able to make small mutations directly in the antigen binding site of the BCR which get expressed in the daughter cells of a rapidly proliferating cell these changes in the variable region change the Affinity or strength that the BCR has for its antigen as antigen becomes limited B cells with the lowest Affinity will die off first making it so that only
those B cells with the strongest affinity for the antigen remain this process is called Affinity maturation helping current and future clinicians Focus learn retain and Thrive learn more