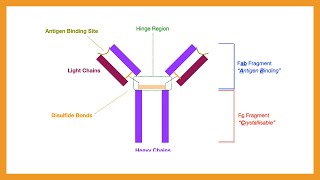
[Music] hello and welcome back to immunology the war is over episode three as promised in this episode we're going to take a deeper look at those interactions between the t cell and the antigen presenting cell we're going to find out exactly how those co-stimulatory molecules work and on top of that we're going to check out some of the biological agents which have been specifically designed to block these and these agents show up everywhere in oncology rheumatology dermatology and transplant medicine and of course in our exams so if you plan to practice medicine anytime in the
21st century you would be well advised to pay close attention to this episode now we are going to be meeting a few co-stimulatory characters and to help us remember these concepts i want you to try and think about the t-cell like it's a machine say like a car on that t-cell we have the ignition switch or the on switch also known as cd28 next we have the accelerator pedal cd40 ligand when cd40 ligand is pushed it will ramp up t-cell activation and lastly we have the brake pedals ctla-4 and pd-1 these are like the off
switches for the t cell now on the antigen presenting side we have molecules which are designed to press all of these buttons in a set order i want you to imagine that the antigen presenting cell is the driver of this t cell car it's going to start the t cell accelerate the t cell but then also stop the t cell b71 and b72 also known as cd 80 and 86 on the antigen presenting cell are like the keys in the ignition of the t cell they bind to cd28 turning the t cell on once the
t cell is switched on it then sends a signal back to the antigen presenting cell to let it know the activation has occurred you can imagine that it's like that sound your car makes when it's ready to go and when we hear that sound we hit the accelerator to put that car into motion and the antigen presenting cell does the exact same thing when the antigen presenting cell recognizes that the t cell has switched on it changes its intracellular signaling in order to place lots of cd40 molecules on its surface and the cd40 molecule is
going to press on cd40 ligand the t cell accelerator pedal and at the same time as the antigen presenting cell ramps up cd40 on its surface it also ramps up mhc molecules to further consolidate antigen presentation and get those t cell receptors fired up so now there are lots of accelerator pedals being stimulated on the t cell and lots of antigen presentation which boosts the signal at the t cell receptor t cell activation is now very much underway the vehicle is in motion but then just like you can turn a key to start a car
you can also turn that same key in the opposite direction to stop the car and so b7 1 and b7 2 whilst they are indeed the on switch for the t cells when they bind to cd28 they are also the off switch for t cells when they interact with the brake pedals ctla4 or pd1 so b71 and b72 are both the on and off switch for t cells depending on what they are binding to depending on which buttons they press okay so let's see how that works in real time an antigen presenting cell rocks up
at the lymph node has the cuddle party we saw in episode two until eventually a t cell comes along that matches the antigen being presented this binding of the t cell receptor to the mhc antigen complex is known as signal one which anchors the two cells together and is otherwise known as a stop signal now it's time for signal 2 which involves those co-stimulatory molecules it's worth pointing out that initially there are only activation molecules present on the surface of these naive t cells their inhibitory molecules or brake pedals will come later so at the
start b7 doesn't have anything else to bind to except cd28 and this forms the key in the ignition sparking off the t cell this also causes a change within the antigen presenting cell which ramps up antigen presentation and places lots of cd40 molecules on the surface these cd40 molecules press on those cd40 ligands the t cell accelerators and the t cell is now very much up and running meanwhile inside the now activated t cell there are stimulatory pathways happening which increase the production of interleukin-2 and h-receptor remember interleukin-2 as to the t-cell what cups of
coffee are to me the cell is making its own fuel for its own proliferation but equally as those stimulatory pathways get underway there are inhibitory molecules being produced and inserted onto the t cell surface and these inhibitory molecules are the brake pedals ctla4 and pd1 now this is where it gets real clever b71 and b72 actually bind to these brake pedals with higher affinity than they do to cd28 so they bind to the off switch much more easily than they bind to the on switch and so when these brake pedals appear on the surface of
t cells b71 and b72 shift their attention towards those brake pedals and away from cd 28 preventing further t-cell activation this also reduces the amount of adhesion molecules on the cell surface so the t cell and the antigen presenting cell start to lose grip on each other and a really funny thing that can happen at this stage is something called trans endocytosis it's kind of like a little t cell tantrum the t cell literally reaches out grabs the b7 on the antigen presenting cell ingests it and destroys it and with that the cuddle party between
the t cell and the dendritic cell comes to an abrupt end so that's how the co-stimulatory molecules work now let's take a look at some of the monoclonal antibodies which work to manipulate these processes in our clinical practice drugs developed to block coastal military molecules can work in two ways depending on the goal you're trying to achieve if you want to immunosuppress someone in the setting of transplantation or autoimmune disease the goal is to stop the t cell from being activated in the first place in other words you don't want the key in the ignition
switch at all if on the other hand you want to create a colony of activated t cells which fight cancer then you're absolutely going to let those t cells become activated and then you're going to keep them activated by blocking those brake pedals and drugs have been developed to take t-cells down each of these pathways let's start off with blocking the t-cell from the get-go say in the interest of organ transplantation or autoimmune disease drugs such as baladacept and abatacept are designed to stop the t cell before it gets started and the only way to
do this is to block that key from turning on the ignition switch in other words we want to block the b7 molecule from binding to cd28 that is the goal and drug developers understood that b7 much prefers to bind to ctla4 than to cd28 so they took advantage of this they took a bunch of ctle4 molecules and attached them to components of antibodies to make a fusion molecule these ctla fusion molecules bind to b7 and block its function and this is genius so infusing bladder sept is like infusing a whole bunch of brake pedals that
bind to b7 on the antigen presenting cell and stop it from activating the t cell so that's how these drugs work but where can we see them in our clinical practice a badasept is typically used in the treatment of rheumatoid arthritis whilst bilatercept which was designed to bind more tightly to b7 than a badassept is used in transplant settings in some countries now some of you might be wondering why do we block b7 instead of cd28 wouldn't it be better to just jam up the ignition and totally mangle the on switch and this has been
tried but unfortunately so far the anti-cd28 therapies that have been developed actually stimulate cd28 rather than blocking it so the complete opposite of what you'd be hoping for so at the moment infusion of brake pedals which bind to b7 is the better option but as we mentioned before there are some clinical scenarios where we might want t-cells to be activated in order to combat cancer cells in this setting we want the t cell response to be profound and for those t cells to go after and destroy every last tumor cell without mercy we do not
want to switch off our t-cells as mother nature intended no no we want to override mother nature's offswitch by getting rid of those brake pedals sounds dangerous but we're talking about fighting cancer here so whatever it takes so in this scenario we want t cells to become activated we allow the b7 to switch on the t cell via cd28 but remember that once a t cell is activated it will start to place its own brake pedals onto the surface these would normally steal away b7 from the ignition switch and reduce t cell activation now this
is the part we don't want and so as those brake pedals emerge we want to block them and we do this by infusing monoclonal antibodies which binds to these brake pedals and render them defective now all b7 can bind to is cd28 and so the t cell has a very active on switch but a very unreliable wonky off switch and drugs which work in this way are collectively known as the checkpoint inhibitors so the checkpoint is referring to mother nature's offswitch the insertion of those brake pedals following t cell activation so a checkpoint is mother
nature's way of keeping the immune system in check and because we have two different brake pedals we have two groups of checkpoint inhibitors the ctle4 inhibitors and the pd-1 inhibitors perhaps the most famous ctla4 inhibitor is epilimumab which is used to treat melanoma as well as some other cancers an example of a pd1 inhibitor is nivolumab which is used to treat both solid organ malignancies and lymphomas but these checkpoint inhibitors do have their downsides when t cells are unregulated it poses a risk of autoimmune disease and this is a typical adverse effect of these drugs
autoimmune side effects range from mild to severe and can affect numerous organs and tissues around the body clinicians prescribing these drugs need to watch out for these complications and treat them promptly so someone on these drugs who develop say diarrhea you have to think is this garden variety infective diarrhea or is this a potentially life-threatening bowel inflammation manifesting as diarrhea but thankfully even when these more severe autoimmune complications occur they tend to respond really well to systemic glucocorticoids and having an autoimmune reaction with these drugs is double-edged at the very least it tends to mean
that the drug is doing a good job of t cell activation and so in some instances these autoimmune manifestations have been associated with an improved treatment response in terms of managing the underlying malignancy so that was co-stimulatory molecules and the drugs which block them i hope you enjoyed this episode as much as i enjoyed creating it don't forget to test your knowledge in the mcq section over at reno tutorials by christine barker i'll leave a link in the show notes and of course tune in again soon for episode 4 when we will be stepping away
from tea helper cells and bringing cytotoxic t-cells into the spotlight i'll see you there you