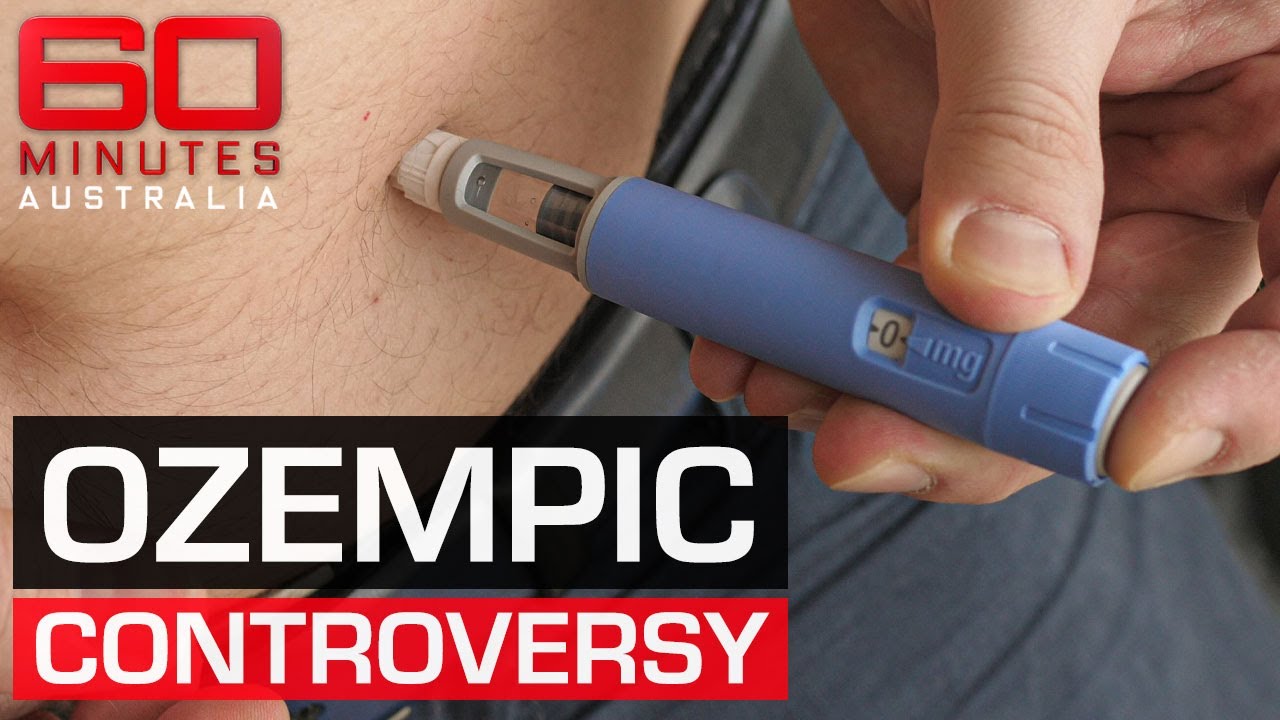
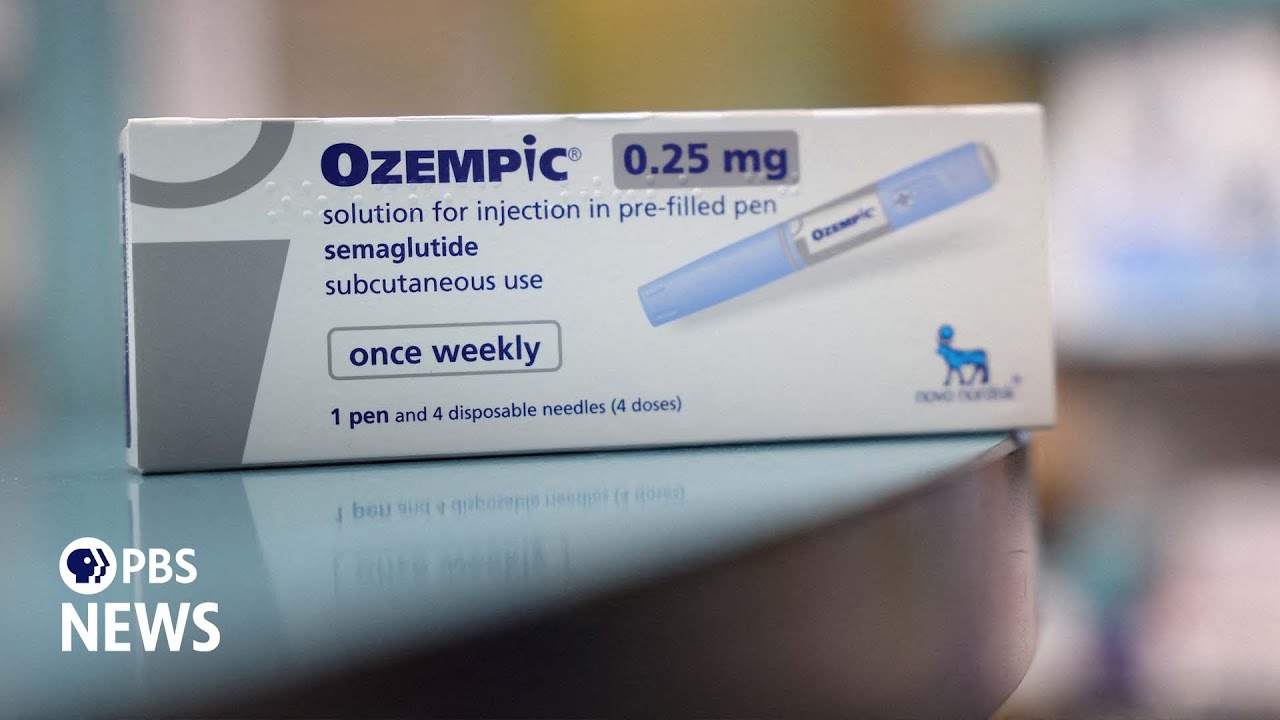
[Music] here's your money briefing for Wednesday May 17th I'm J.R Whalen for the Wall Street Journal ozempic and similar drugs that have hit the market in recent years may be able to promise to help people lose weight but insurers are often reluctant to cover the cost of drugs that can list as 900 or more per month wsj reporter Anna wilda Matthews joins us to discuss the best ways to get your health plan to pay for your prescription so Anna how do these medications work and who are they geared toward well ozempic isn't a category of
drugs that work by mimicking the effects of a naturally occurring gut hormone which is called for short glp-1 glp-1 drugs contribute to weight loss by suppressing appetite and making you feel full sooner when you eat ozempic and munjaro are both geared toward people with type 2 diabetes the FDA has approved them for that use what Govi is explicitly approved by the FDA for weight loss for treating obesity although the labeling on the drug actually indicates that it's not just for a person who maybe wants to lose a few pounds it's really for people who are
in the category the clinical category of obesity which means they have a BMI of 30 or more or they can have a BMI of 27 or more and then also have a related health condition such as high blood pressure so these drugs are geared toward people with weight problems for different reasons well so specifically munjaro and ozempec are approved treat diabetes they are not approved to treat obesity so they are really to help with diabetes with blood sugar issues with Govi although it has the identical active ingredient to ozempic is explicitly approved for weight loss
what steps would someone take to start treatment with these medications well the first thing is is obviously to see a doctor these are prescription medications and people can't just you know go to the drugstore and pick them up and it is also true that these medications can have a significant side effects and we are told by by The Physicians we interviewed for the story it is important to be under the care of a physician both when you seek to get the drug and once you're on it if your doctor does agree that one of these
drugs is a good fit for you that you could benefit typically then there's a process that you and your doctor will have to go through seeking approval from your insurance company that's not always the case but it is increasingly and often the case now on social media and on the TV commercials the Splashy headline is that these drugs can help people lose weight why has it been such a challenge for insurers to cover weight loss drugs and programs in the past well it is true that a lot of employers and a lot of insurance plans
don't cover drugs explicitly for weight loss some do but many don't in the past it has sometimes been considered and I will put air quotes around this a lifestyle or again air quotes cosmetic issue that thinking is definitely evolving in the medical establishment Physicians often now consider obesity not again quote lifestyle issue but really a health issue and a medical condition that needs to be treated but again in the past a lot of insurance plans haven't treated weight loss drugs as something that was vital to cover now if a doctor prescribes the drugs is that
the green light needed for an insurer to cover the cost it's often not the only green light so if a physician prescribes one of these drugs again typically there's a process that is kicked off The Physician will also often have to apply for authorization for the drug to be covered by the insurance plan often called prior authorization so there may be a form that the physician has to fill out or perhaps a letter that they might have to write typically the health plan is looking for evidence that proves that you really do need the drug
if you have type 2 diabetes and you're seeking access to ozempic umunjaro you may have to show first of all that you do have diabetes and then in some cases they might want evidence that you have already previously tried a different drug for diabetes and perhaps not gotten the results that you were hoping for if you don't have diabetes you probably would be seeking with Govi because often they're not going to give you the diabetes medications if you don't have diabetes and in that case they'd be looking for things like whether you meet the conditions
that are spelled out in the label of wagovi so again that would typically be having a BMI of 30 or higher or a BMI of 27 or higher along with a related health condition such as high blood pressure in addition there sometimes looking for other things like you've tried other efforts at Weight Loss often through a structured program and if a health plan does provide coverage of ozembic wigovi or a similar drug does that mean the patient is clear of any out-of-pocket costs it depends on the health plan as we all know that any of
us who've had more than one Health Plan knows that can be completely variable how much you have to pay out of pocket for the same treatment depending on what employer you're with or what insurance plan you have but it can vary it can be at just a flat cone payment like we often experience for drugs but these are pricey drugs and employers are leery of the cost both of the drugs for each patient and the number of patients who potentially could be eligible for them at some point so we did hear that anecdotally that some
employers are starting to ratchet up the out-of-pocket cost for patients who are getting coverage for these drugs so instead of perhaps a flat copay a plan might ask you to pay a co-insurance which means a percentage of the cost of the prescription Ana this seems like a new wave of drugs to address different ways that people put on substantial amounts of weight are we at a point now that insurers are going to have to maybe change their ways well it's maybe too soon to tell one key thing to keep in mind is it's not just
insurers it's often employers so depending on the size of the employer most large employers for sure are self-insured which means they do decide they'll decide what what they cover and what they don't there are not federal regulations requiring that weight loss drugs be covered so that gives flexibility we did hear that employees who are seeking these drugs and feel that they they really need them and whose Physicians feel they really need them some do appeal to their and their employers and insurers saying you know I really need this and you need to cover it they
ask for either a change in policy or for an exception for them and this can work although it's not clear how often it does but over time it seems possible that more and more employers will see pressure from employees seeking access to these drugs and will again come under sort of some pressure from their own workers to change policies when they when they don't cover them that's Wall Street Journal reporter Anna wilda Matthews and that's your money briefing I'm J.R Whalen for the Wall Street Journal [Music] foreign