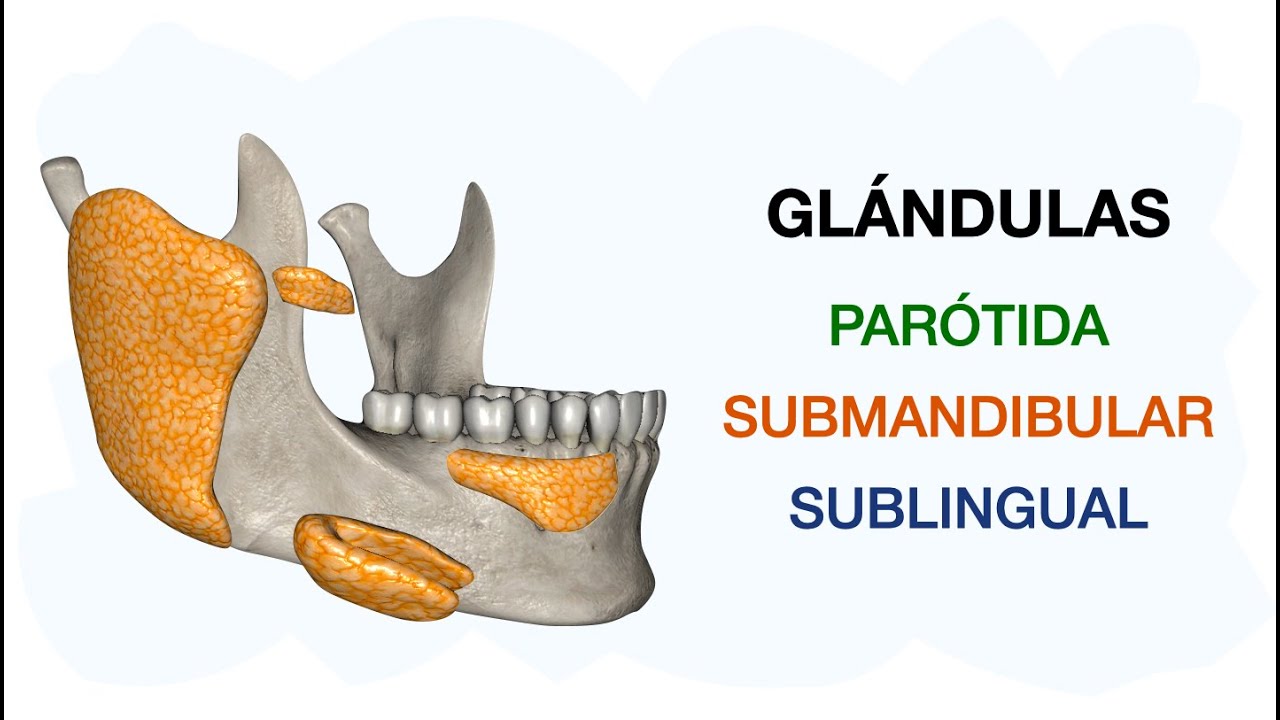
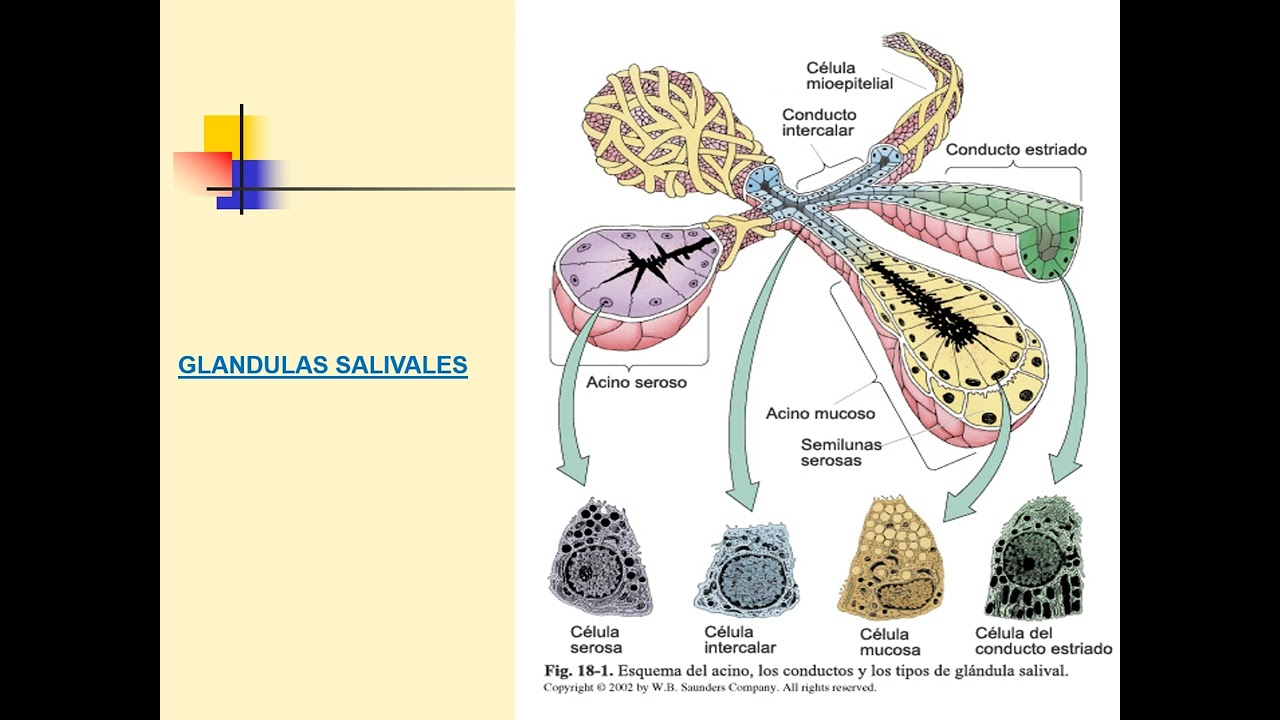
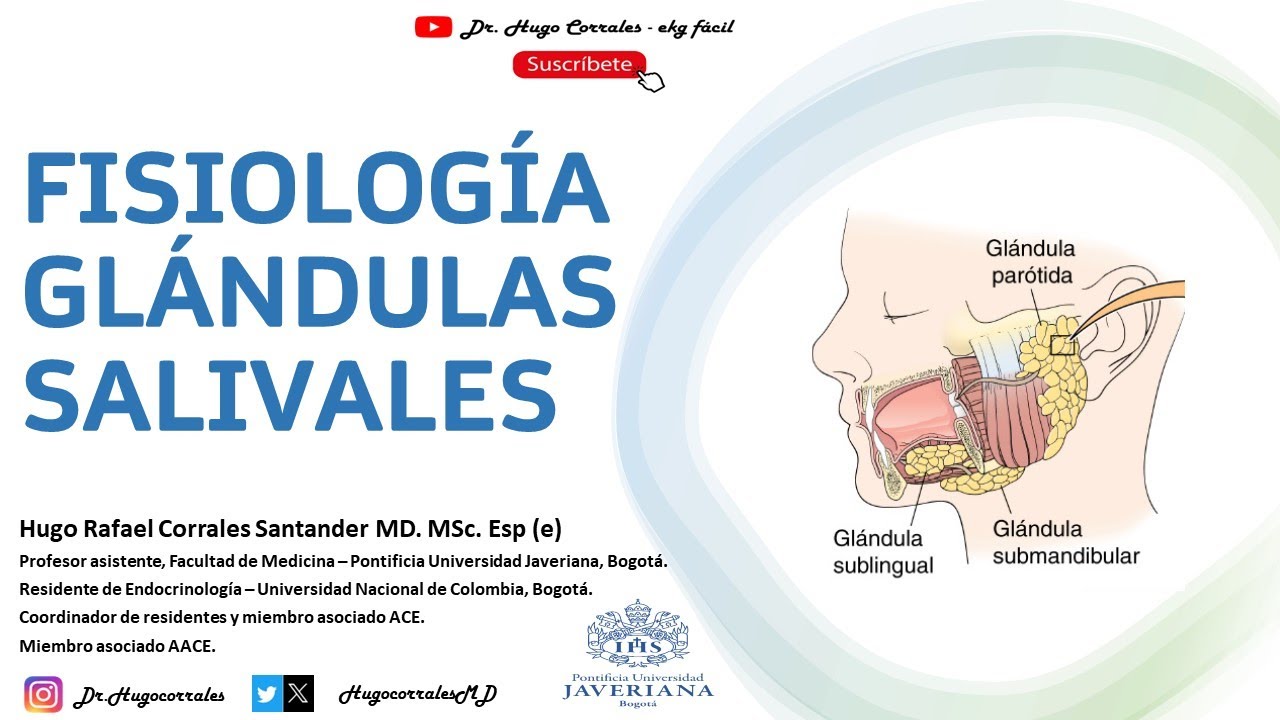
My dear listeners, welcome once again to another new anatomical video, my name is Juan José Sánchez and today we will talk about the major salivary glands, in general the salivary glands are divided into two large groups: minor salivary glands that are not studies of macroscopic anatomy since they are glands that produce saliva but that are seen under the microscope and are studied in histology that are found along the buccal mucosa of the reel at the level of what is the palate, at the level of what is It is the floor of the mouth. Today we will talk about three large glands that make up the major salivary glands, so we will first talk about the largest of them, which is the parotid gland, then we will talk about the submandibular gland, also called the submandibular gland, and finally we will end by talking about what It is the sublingual gland so these are the three glands that are within this group of major salivary glands. So without wasting any more time let's start talking about the parotid gland, but before that I am going to explain the anatomical location of the parotid glans, which is at the level of what the parotid region is, this parotid region is a region that is located within what is the anterior triangle of the neck, okay?
and it will have as its anterior limit what is the ascending root of the lower jaw, as its upper limit what is the EAC, that is, the external auditory canal, as its posterior limit in the most superior part it will have the mastoid process, in the The most inferior part of the part, let's say of the posterior limit, is the anterior edge of the sternocleidomastoid muscle, while its lower limit will be the posterior digastric muscle. So in that region that most of the parotid gland is located, however, the parotid gland also has a part that is on the face in front of what is the lower jaw, so the parotid gland or parotid gland is a gland which is first surrounded by a membrane, by a fascia, we are going to call that membrane parotid fascia as you see here, you also see that superficially after we section the skin it is in contact with the skin it will be directly in contact with what which is the platysma muscle or cutaneous muscle of the neck, then saliva is nothing more than a mixture of secretions, saliva is a mixture of serous secretions and mucous secretions. So throughout this video I will talk to you about what type of secretion each gland provides, so the parotid gland is going to provide a secretion that is almost purely serous, some books say that it is only serous, okay?
That parotid gland will have a shape like an inverted pear or an inverted pyramid, the apex will be found towards the bottom in a region that is between what is the sternocleidomastoid muscle and what is the lower jaw, while The base like an inverted pyramid is superior looking towards what is the zygomatic arch, in addition to this the parotid gland will have three faces; an external face that is exactly what we are seeing in this image, okay? To explain the other two faces we are going to make a cross section at the level of the mastoid process that goes through this middle that is here which is the facial nerve, so this is the image so that you understand this is the mastoid process and this is the lower jaw, remember that it was a transverse cut that I also cut the lower jaw, so this face that we see here would be its external face, which is what we see right now, that external face is the one that will be in contact with the skin and It will be in contact with the cutaneous muscle of the neck, and it is also said that on this external surface there is a group of lymph nodes that are immersed within the parotid gland. Then we have the anterior face, which is furrowed.
See that it has a furrow that is formed by the ascending branch of the lower jaw. This means that we can subdivide this anterior face into two lips, this one that you see in blue is going to be the lip. external then of the anterior face and this one that you see in red the inner lip medial lip of the anterior face, do not forget that from this anterior face it is then separated or these two lips form the groove left by the lower jaw, that anterior face will be in close relationship, specifically its external lip with the masseter muscle while The inner lip will be in contact with the medial pterygoid muscle; some say that this portion even fits between the medial pterygoid and the lateral pterygoid.
While the third face then I already talked about the external of the anterior, the third face the parotid gland is going to be the posterior face which is the face then that is going to be in contact with the mastoid process, it was going to be in contact with the muscle sternocleidomastoid which is this face that you see here and in the most superior part that posterior face is in contact with what is the external auditory canal. So there are a series of vascular structures, nervous structures that pierce this parotid gland. Let's start first with the nervous structures and without a doubt the most important structure that pierces my parotid gland is precisely this nerve that is here, which is the seventh pair.
cranial, that is the facial nerve even, see that the facial nerve when it pierces it branches inside it giving what is known in anatomy as the goose's foot because you see that there are many ramifications of the facial nerve, so that is why it is very important In parotidectomy, which is the operation by which the parotid gland is removed, preserving or trying to preserve the facial nerve and not touching it because we are going to cause injuries to it, we are going to see that there will be, let's say, a loss of muscle function. of the facial expression, which are the muscles innervated by this goose foot, in addition to this we are going to see that this facial nerve, which is the one you see here, pierces my parotid gland, first it enters through what is its posterior face and then It comes out on the anterior side but specifically on the internal side it is in the anatomy or the course of the facial nerve as such at the level of what is the parotid gland or parotid gland, in addition to that see this nerve that is here which is the auriculotemporal nerve , this auriculotemporal nerve gives a branch of the mandibular nerve or lower maxillary nerve, which in turn is a branch of the fifth cranial nerve, which is the trigeminal nerve. What I want you to know is that this auriculotemporal nerve pierces what is the parotid gland, which refers to very important vascular structures.
Here we see the external carotid that perforates the parotid gland. If you have already studied what the part of the neck arteries is, you will know that the external carotid gives two terminal branches: one is the superficial temporal one that we see here and the Another is the internal maxillary artery, in this image it looks much better, we dissect the parotid gland and we see that the external carotid gives its last branches, which is the internal maxillary that goes inside the lower jaw and this is the superficial temporal artery. , then if the external carotid pierces the parotid gland it is assumed that then its two terminal branches will also begin in the thickness of the parotid gland, both the internal maxillary and the superficial temporal, in addition to this see that there is a branch of the superficial temporal artery that is called transverse artery of the face because this transverse artery of the face also pierces my parotid gland, now the places where they pierce are different because this superficial temporal artery specifically is coming out from the base of what is the gland parotid artery, but what is the internal maxillary artery?
How does it go inside the lower jaw? If it is going to come out specifically through the inner lip of the anterior face, while the transverse face, remember that it comes from the front. What the lower jaw is, so that it is going to come out is through the external lip of the anterior face and what the venous structure refers to, see that there is a vein in which it is the same or let's say it is similar to what it is.
the superficial temporal artery which is the superficial veins, this vein also pierces what is the parotid gland. Now I pause here because this vein here is the jugular vein, external this jugular vein Although you see here that it is forming outside the parotid gland, many authors agree that the external jugular is formed in the thickness inside the parotid gland, so I have to assume that the two veins that form my To the external jugular vein they also have to pierce the parotid gland and that is the posterior auricular vein which is this one and this one which is the retromandibular vein, so they are venous structures that also pierce the parotid gland, now this parotid gland produces its saliva, But because it is an exocrine gland, it needs an excretory duct that carries saliva to the mouth. That duct is the one we see here shaded in black, which is what we call the sternum duct or simply the parotid duct.
It is a duct that does not It carries lymph or anything like that but it simply transports saliva, it will be lateral to the masseter muscle without touching it, it measures five centimeters and then pierces the buccinator muscle, okay? Once it pierces the buccinator muscle, it opens out, it is said to be at the level of the upper second molar, the second upper molar colloquially, and there is a hole that is the one we see here, which is what we call the parotid papilla or in anatomy the papillae. They are also called caruncles, so the same thing I say parotid caruncle is the place where the parotid gland empties, which is the one that provides the greatest amount of saliva, the innervation that I have a diagram for you to understand.
Let's start first with the parasympathetic innervation. , this nerve that you see here is the fifth cranial nerve which is the trigeminal, this one that you see here the facial nerve and this one that you see here the glossopharyngeal, then the parasympathetic comes through the glossopharyngeal nerve, that glossopharyngeal nerve gives a nerve that is called tympanic branch, listen well, that tympanic branch forms a plexus at the level of the eardrum but does not innervate it, it is called tympanic because it passes through there and after that tympanic plexus a nerve comes out derived from the plexus which in turn derives from the tympanic branch that It is called the lesser superficial petrosal nerve, this lesser superficial petrosal nerve is what carries the innervation of that glossopharynx to this ganglion that you see here, which is the otic ganglion, so up to there they are preganglion fibers because they are fibers that come but have not done so. synapses, that's why you see them there without a point, they are not pointed but rather a continuous blue line.
Once there, those pre-ganglion fibers have already made synapses at the level of the otic ganglion, a nerve comes out that joins this nerve, which is the nerve. auriculotemporal, is a branch of the mandibular nerve which in turn is a branch of the trigeminal, so through that auriculotemporal nerve, it reaches the parasympathetic innervation to what is the parotid gland, which are secretomotor fibers that you already know derive from the glossopharyngeal but what they end up using is the temporal auriculonerve, some authors also say that there is a union between what is the seventh nerve, which is the facial along with the glossopharyngeal, so it is said that it also provides fibers that help innervate the glossopharyngeal, That's what sympathetic innervation refers to, but the sympathetic innervation, you already know that the spinal segments D1, D2 come, they ascend throughout the cervical sympathetic chain, preganglionic fibers, see that they have not made synapses, once they touch the superior cervical ganglion, they come out the sympathetic postganglionic fibers , which are the ones that will provide the sympathetic innervation to the parotid gland, then we continue with what is the submandibular gland, previously called the submandibular gland, this submaxillary gland will be found or will be made up of two portions: a portion that we have called the body of the submandibular gland or simply the greater or superficial portion and one that is located deeper than the next deep portion or minor portion. within the type of saliva that the submandibular gland produces is a type saliva or a mixed type secretion, a mainly waxy secretion but that has a part of mucous secretion, then this submandibular gland these two portions are going to join at the edge posterior of this muscle which is the key muscle of the submaxillary gland which is the mylohyoid muscle, she hugs the mylohyoid muscle, then she is going to have see here how its deep or lesser portion joins at the posterior edge of this muscle that the mylohyoid with the superficial portion which is the greater portion or simply body of the submandibular gland, then see that it will be made up of three faces, an inferior face that is a face that will be in contact with the platysma muscle will be in contact with the submaxillary lymph nodes and will be in contact with this vein that is very important than the one that I will explain later that collects venous blood from the submandibular gland, which is the vein this is called the submandibular vein, sorry with the facial vein.
Now, after this lower face there will be a face that will be in contact with what is the internal face of the lower jaw, that is the external face, listen well, the external face of the submandibular gland, these already know that it is in contact with what is the lower jaw, in fact it even makes a fossa that in anatomy is known as the submaxillary fossa, so look here so you can see how the facial vein collects blood and is related to the face inferior of what is the submaxillary gland and finally there is an internal face that is in contact with what is the mylohyoid muscle, that is what we call internal face in addition to being in contact with the mylohyoid muscle it is also It says that it is in contact with the hyoglossus muscle, which is not seen in this image, so that submaxillary gland also has an excretory duct through which it secretes its saliva. That duct is the one you see here in green, which is the medial vasa and is also five centimeters long. , it passes medially or internally in what is this gland, which is the sublingual gland that we are talking about right now and empties at the level of what is the lingual fold or the lingual alveoli fold, then there it empties through a duct that is lateral to what is the frenulum of the tongue , which is what we call the forgiveness duct.
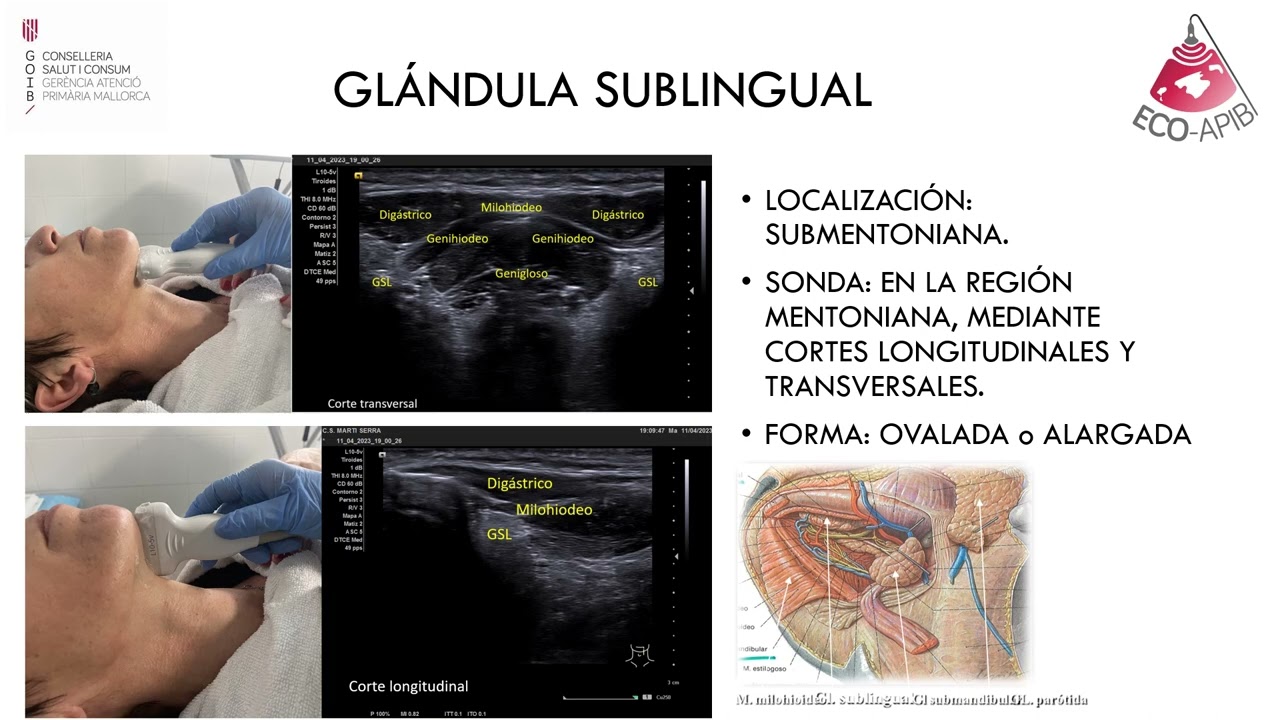
The duct is called the submaxillary duct or also called Wharton's duct and the hole through which it empties is what we are going to call the submandibular papilla or we will simply find it with the name of the sublingual papilla as you see it in this submandibular image or caruncle. sub maxillary sorry, it is called sub maxillary papillae or sub maxillary carucula, now the irrigation in venous drainage is extremely easy, the irrigation will be given by what is the facial artery while the venous drainage will come by what is It is the facial vein, then we are going to talk about the sublingual gland which is the last one that we need to talk about, this sublingual gland remember that there are two glands, one on each side of these three that we have talked about are paired glands, this lingual gland goes to have several relationships, it will be found below between what is the hyoglossus muscle while sorry, mylohyoid while above it will be found with what is the mucosa that lines the floor of my tongue, now both sub glands jaws are separated both on the left side and in this image with the one on the right side, they are separated by a muscle that is not seen in this image, which is the genioglossus muscle. This muscle separates both sublingual glands that already have a close relationship.
with what is the hypoglossal nerve that is above it, we do not see it in this image and with what is the lingual nerve that we see in this image that is below it. Now in this gland here we see the relationships well Of this muscle that we see here, it is the genioglossus muscle that separates both sublingual glands, the one on the left side and the right side, and as I told you right now, they are located between what is the floor of the mouth and what is the mylohyoid muscle of the type of secretion of the sublingual gland is a clearly mucous secretion glands, now this sublingual gland will secrete its saliva not through a single duct as its two predecessors did, but rather it has a series of ducts that are 10 to 30 that It flows into it along the entire length of the lingual alveoli fold, along the floor of the mouth there are many ducts, there are 10 to 30 and these ducts are called sublingual ducts, while each hole that opens or through which it opens into what we call sublingual papillae or caruncles, which would also be 10 to 30, there are some sublingual ducts that join the submaxillary duct and drain with it, but most drain only separately, as we see in this image, here we see at this level what the sublingual papillae are and these little circles that you see here on the sides of what is the frenulum of the tongue are the mouth ducts of the submandibular gland, the famous Wharton duct, now the irrigation and venous drainage of this sublingual gland that is dissected here is irrigated by a branch of the lingual artery which in turn is a branch of the external carotid which is the sublingual artery which is this one that you come here and your venous blood comes collected through the sublingual vein that gives into the facial vein and the facial vein ends up draining into the internal jugular vein, now the innervation of both glands, I am referring to the submaxillary gland and the sublingual gland, is In the same, both are innervated by the lingual nerve but what happens the lingual nerve is not the one that carries the fiber itself or the origin of those fibers that innervate the state gland, this nerve that you see here is the facial nerve, which is the seventh cranial nerve that facial nerve of a branch that you can see here, that gives it inside the skull that is why we do not see it, here we see how the same branch of the facial nerve is as this nerve branch that is called the chorda tympani nerve and This chorda tympani nerve joins what is the lingual nerve, which in turn is a branch of what is the fifth cranial nerve, which is the trigeminal nerve, and this lingual nerve is the one that ends up carrying the pre-ganglion fibers that derive from the facial nerve. You know, through the chorda tympani nerve to this ganglion, the submaxillary ganglion and this submaxillary ganglion, which will carry the post-ganglion fibers for both the submaxillary gland and the sublingual gland, the sympathetic innervation also comes from the thoracic segments.
t1 t2 ascends throughout the cervical sympathetic chain and once it reaches the superior cervical ganglion, the post-ganglion sympathetic fibers leave and go to the submaxillary gland and the sublingual gland. So friends, this has been the entire video, don't forget to like the thumbnail you see below, share the video and subscribe to my channel so you can receive more videos like this one.